Dr. Friedman's Office: (210) 880-3000
Dry Eye Syndrome

Redness, itching, burning, and irritation of the eyes are all common complaints. They can be caused by any number of reasons such as allergies or exposure to environmental problems like smoke, wind, etc. Still, some people start to develop these symptoms without external causes. For these people, the problem might be underlying dry eye syndrome.
The eyes are different than most surfaces of the body. They have to be kept constantly moist by your tear film. That said, the tears are actually a very dynamic substance. They are composed of three layers. The topmost layer is actually like an oil slick. It is a very thin layer of lipid (fat) that comes from the glands on the eyelids. Much like an oil layer on water, it protects the underlying watery layer from evaporating too fast. Next, the majority of the tears are (as you would suspect) water, mixed in with enzymes, antibodies, and all sorts of good substances to keep the surface of the eye moist and healthy. Finally, at the bottom, is a layer of mucous. It is really thin and comes from the skin of the eye known as the conjunctiva. It helps the watery layer stick to the surface, filling in all the nooks and crannies that need to be filled.
When any one of these layers is not at its best, the tears do not work as efficiently as they should. Ophthalmologists like to divide tear film problems into one of two main causes: 1) aqueous tear deficiency (when the watery layer is not working) or 2) meibomian gland dysfunction (when the lipid layer is not at its best).
Let’s tackle these one at a time. If your eyelid glands are backed up (there are about 20-40 of them on either lid), then the oils cannot get out and coat the surface in one even sheet. Think of it as the difference between oil and butter. Hard oils do not spread easily whereas liquid oils are easier to spread across a surface. People without a good oil film on their tear surface have the underlying water evaporate too fast, thus leaving the eyes dry. Sometimes, the oils get so hard that the glands get backed up and inflamed causing a stye (this is discussed in another section, so feel free to come back to this). Bad oil glands can be due to any number of reasons including hormonal changes (specifically in adolescence and after menopause) or infection from surface bacteria.
If, on the other hand the glands responsible for the water part of the tear film are not producing enough tears, then there isn’t enough water to go around no matter what. This can happen for any number of reasons including inflammatory disorders (e.g., Sjögren’s syndrome, sarcoidosis, lupus), hormonal changes, or even dry eye syndrome itself (yes, chronic eye inflammation actually causes you to produce less tears).
So what do you do if you have the symptoms of dry eye? Although you can probably start many of the treatments at home, it would also be a good idea to see an eye doctor just to make sure that it is not something else causing the irritation or burning. There are many causes for these eye symptoms including allergies, infection, or underlying inflammatory disease. If after consulting your eye doctor you are diagnosed with dry eyes, then you will likely be started on a step-wise approach to battle this problem.
For people with eyelid inflammation (also known as blephritis), the goals are to break-up and thin out the oils. The first step to this is to clean the eyelids. Much like you would put soap into a greasy pan to break up the oils, a good treatment for blephritis is actually washing the eyelids. I currently recommend taking a mixture of “no-tears” baby shampoo and warm water (half and half) and applying it to the eyelids twice a day. This can be done with a cotton swab or the fingers (just make sure you wash your hands first, obviously). Some other ophthalmologists will recommend using eyelid scrubs specifically for blephritis or even makeup removal pads. Any of these have the potential to work. Find the one that works for you.
Another good recommendation is to put a warm washcloth on the eyelids 2 times a day for about 5 minutes at a time. This does not need to be scalding hot. The purpose of this is to heat up the oils. You should also gently massage the eyelids underneath. Basically, think about melting butter and spreading it out. That way, you end up with a nice oil slick across the eye surface. This should be done 2 times a day as well.
As for replacing the lost water, the first step to treat aqueous tear deficiency is trying artificial tears. There are many over-the-counter options available at most grocery or drug stores. That said, here is my advice on how to find the right one . . . find the one that works for you. There are many different substances that can replace tears, and each artificial tear offers something a little different. Since everybody is a little different, some find that certain brands of tears work better for them while others like another brand. It’s ok to shop, and don’t think that the most expensive one is necessarily the best. If you can find an affordable eye drop that fits your budget, use that one.
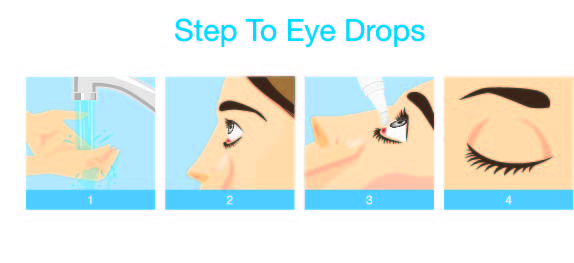
Now, a couple of words of advice. Most artificial tears are meant to be used up to 4 times a day. This is because many of them contain preservatives. When you go beyond the 4 times a day, the preservatives can be irritating to the eye surface and start to get counterproductive. There are preservative free artificial tears, and these are fine to use more than 4 times a day, but be sure to dispose of them soon after opening the little tear off tab because the preservative keeps them from growing things like bacteria.
Also, do not . . . I repeat, DO NOT use drops that tell you they are going to “get the red out”. Ophthalmologists hate these medicines. Here is why. In the short term (say for a talk 15 minutes from putting in the drop), the medicine does a really good job of getting rid of the redness in the eye. Basically, it causes the blood vessels to constrict so they can no longer be readily seen. The problem is that the medicine soon wears off, and a lot of times the redness comes back, maybe even a little worse than before. So, the natural instinct is to put in more “anti-redness” drops. Well, you can imagine what happens next. A bad cycle develops causing the eyes to become more irritated and more red, much to the dismay of the user (and the eye doctor). I will add, that there is a new medication available over the counter that is not within the usual class of anti-redness drops. This is different and goes by the name of Lumify. Results are still pending on the benefits to this drop.

Now, those are all of the very basic treatments for dry eye syndrome: lid scrubs, artificial tears, and warm compresses. I will talk more about severe dry eye syndrome in another section of this website, but hopefully that will get you started. Stay tuned.
Duncan Friedman, M.D.
Ophthalmologist
San Antonio, Texas


