Dr. Friedman's Office: (210) 880-3000
Retinal Vein Occlusion
Did you know that high blood pressure can affect your eyes? Although most of the effects of high blood pressure in the eyes do not cause a change in vision, there are certain instances where a chronic history of high blood pressure can cause significant vision loss.
In this article, we talk about retinal vein occlusions which most commonly result from chronic high blood pressure. This is when a blood vessel leading out of the eye becomes blocked.
Imagine that the blood supply to the eye is like an interstate highway; there is only one major road in and one major road out. Blood only has one major path into and out of the eye to supply the retina. After years and years of high blood pressure, the walls of the central retinal artery (the road into the eye) become very thick. The artery can push on the walls of the central retinal vein (the road out of your eye). If the artery becomes so thick that it closes off the vein by compressing it, no blood can get out of the eye. Like a bad accident on a highway, this causes a ton of traffic to back up into the eye which manifests as bleeding in the retina. When this happens, the retina starts to undergo serious damage because it no longer has good blood flow. This is known as a central retinal vein occlusion (CRVO).
When people get a CRVO, they usually experience a sudden, painless, large amount of vision loss in one eye. As more and more blood gets backed up in the eye, it can cause swelling of the center of vision (known as the fovea). This causes further blurring in the central vision.
There are many tributaries that all flow toward the single, central retinal vein. In a less severe case, one of these tributary veins can get “kinked” in a similar fashion by the artery running next to it. This is known as a branch retinal vein occlusion (BRVO). All blood trying to leave the eye along this branch gets backed up and can leak into the retina. If it is close enough to the center of vision, it can also cause visual loss due to swelling of the fovea.
If you experience any sudden visual loss in one eye, it is important to have an eye doctor examine it and determine the cause. CRVO and BRVO are one of many causes for these symptoms, and an eye doctor can help diagnose this problem.
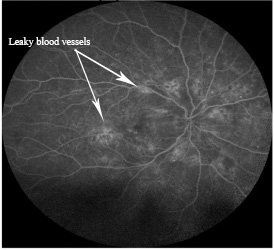
When you are seen by your eye doctor, they will likely test your vision, your eye pressure, and your peripheral vision as well as give you a thorough eye exam. They will also likely run a couple of imaging tests to examine the retina. The first common test is called optical coherence tomography (OCT) which helps determine if the center of vision is thickened and causing visual loss. Another common test is a fluorescein angiogram. This is a dye based test that allows an eye doctor to see how blood is flowing through the back of the eye. If a patient has a retinal vein occlusion, the dye circulates more slowly due to the blockage and shows the presence of leaking blood vessels.
If the fovea is found to be swollen, there are treatments available that can preserve vision and even regain some vision. When a retinal vein occlusion occurs, the retina starts to produce a chemical messenger called vascular endothelial growth factor (VEGF). This chemical asks the retina to start producing more blood vessels in an attempt to deliver more oxygen to the retina (we have discussed this chemical messenger in other diseases as well including diabetes and age related macular degeneration). In order to try and minimize leaky blood vessels in the eye, the goal is to decrease the amount of VEGF. In the past, the mainstay therapy for BRVOs with macular swelling included laser therapy. More recently, two large-scale studies have proven that injecting a medicine into the eye to block VEGF is a more effective means of minimizing the bad effects from both CRVOs and BRVOs. Your eye doctor might choose a series of therapies including anti-VEGF injections, steroid injections, and laser to help treat the vein occlusion. Also, the swelling in the retina does not resolve immediately because it takes time for blood flow to recover. While this is happening, you might require a series of injections/laser to help treat the retina.
In a central retinal vein occlusion, the visual loss can range from “mild” to “severe” levels. The amount of visual recovery is dependent on how poor the blood flow is initially and how quickly the retina regains good blood flow. In a BRVO, the vision is usually only partially affected (either the field of vision above or below the horizon), and recovery is also dependent on how quickly good blood flow is restored to the eye.
There are a few instances where CRVO can cause worsening outcomes. If the blood flow is poor enough, the retina might start to grow abnormal blood vessels at the front of the eye, which is also deprived of oxygen. If these block the drainage system of the eye, you can develop a quick rise in eye pressure known as neovascular glaucoma. This can cause severe pain in the eye and usually occurs about 3 months after the initial CRVO. If this happens, your doctor will likely need to put an anti-VEGF agent into the eye as well as a significant amount of laser to make the abnormal blood vessels go away. Regular checks by your eye doctor can help monitor for any new blood vessel growth that might lead to this unwanted outcome. Visual recovery from these situations can be poor due to optic nerve damage. Although neovascular glaucoma is rare, I have seen it happen a few times.
Ultimately, the best means of avoiding vein occlusions relates back to where we started, by avoiding the effects of long-term, high blood pressure. Prevention is the most important intervention. Good control of blood pressure usually helps avoid the possible development of a vein occlusion. I would also add that smokers are at higher risk as well as people with diabetes. If you are smoking . . . STOP!!! . . . not only for your eyes’ sake, but also for your general health. If you are a diabetic, it is also important to control your blood sugars. This ounce of prevention can help avoid years of future treatment and significant visual loss.
As always, if you have further questions or inquiries, please feel free to send an email to sanantonioeyedoctormd@gmail.com.
Duncan Friedman, M.D.
Ophthalmologist
San Antonio, Texas


